COVID-19 has been around long enough that we are not even counting the waves anymore, but the virus and the tools we have to fight it keep evolving.
And the guidance seems to change just enough with each surge that it can leave even the most diligent among us feeling lost.
Now, more than two years into the pandemic, some parts of the U.S. are seeing an uptick in cases driven by the BA.2 subvariant.
Dr. Celine Gounder is a senior fellow and editor-at-large for public health at Kaiser Health News and a former adviser to the Biden administration. She runs through the latest thinking on everything from at-home tests to isolation times, contact tracing and why we may be repeating the same mistakes we made with other diseases.
This interview has been edited for length and clarity.

Interview highlights
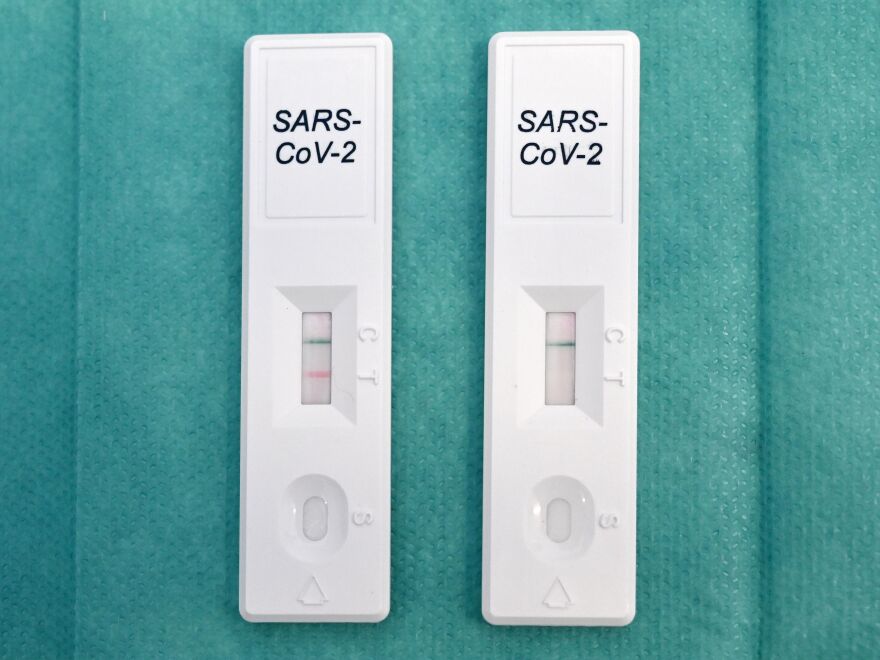
On whether the rapid at-home tests work for BA.2
The rapid antigen tests do work to pick up omicron. This pattern that you see is really similar across all the variants, which is that there is usually a day or two delay between when you might test positive on a PCR versus when you might test positive on one of these at-home rapid antigen tests. But they do work to pick up an infection.
On the expiration dates listed on rapid at-home tests
I organize my tests in my drawer actually by expiration date, so I'm using the oldest ones first. So that's just a small tip there. But the tests probably are good for much longer than they're labeled for. And that's really a reflection of the fact that early on when they were first developed, we weren't quite sure how long they would be good for. And they probably do last probably, you know, in the order of months longer than what they're labeled to be good for.
On when and how to seek treatment if you test positive
To access treatment, you can go to covid.gov and look up where in your area you can access Paxlovid and monoclonal antibodies, what facilities currently stock them, and how you can go about getting that. If you already have a primary care physician, they can also help you navigate that.
Right now, we have a pretty short supply of treatment. And so we're really trying to target that supply to people in whom it would really have the most benefit. People who are young, healthy, who don't have significant symptoms are probably not going to end up in the hospital regardless. And so that's not the best use of that short supply that we currently have.
On isolation times if you test positive
What we're seeing is that people very often test positive for longer than five days. You have maybe about half of people who are negative by five days, but then the other half are positive out to even 12-14 days. And so I think the way to address that is repeat a test. If you're still positive, really try to stay at home. And if you absolutely cannot stay at home, that's a situation where you really should be masking when you're around other people so that you're not infecting others.
On the current state of contact tracing
Contact tracing efforts have largely been dismantled at this stage. And it's become even harder to do contact tracing now, especially if you're trying to use that as a way to prevent onward infection. And that's because the incubation period for COVID has gotten shorter and shorter with each variant. And so with omicron, the incubation period is only two to three days. And so that makes it really hard to try to track down the person that you might have infected and take measures to prevent on onward infection.
I do think if you have been around people, and may have exposed them, I think it's just polite and good form to inform them so that they know they may want to get tested themselves.
On federal funding for COVID measures drying up and whether this is a normal progression
I guess it depends on what you call normal. Is it how we have addressed other diseases and fallen short? Absolutely, it is repeating those same mistakes. We've run out of money to reimburse providers for offering testing to uninsured patients. But it's not just testing. We've also run out of money to reimburse providers for treating uninsured patients, for vaccinating uninsured patients. And it's really unfortunate that we refuse to learn from previous experiences.
I'm not going to tell Congress what to do here. But I think if our goal is to adapt and live with COVID in a way that this is not impacting our social lives or economic lives, our work, then it will mean doing things differently, doing things better, and I hope we will.
The audio for this story was produced by Megan Lim.
Copyright 2022 NPR. To see more, visit https://www.npr.org.